Why Should I Bring my Pet to Willows for Treatment of Osteoarthritis?
Willows is one of Europe’s leading small animal Orthopaedic referral centres treating over 1000 new patients a year. Our state-of-the-art hospital is led by internationally renowned Certified Specialists committed to providing the highest standards of care. Our team of Orthopaedic Specialists have extensive experience of managing thousands of animals with osteoarthritis.
Our Orthopaedic Surgeons are supported by our multi-disciplinary team of Specialists across a number of disciplines including; Anaesthesia, Diagnostic Imaging and Emergency and Critical Care. Willows has a large dedicated team of Nurses and clinical support staff available 24 hours a day, every day of the year to provide the best possible care for your pet.
What is Osteoarthritis?
Osteoarthritis is a very common problem in small animals. It has been estimated that up to half of all dogs and cats will be affected by osteoarthritis at some point in their lives. The condition causes long term degeneration of joints and involves many tissues including cartilage (the joint surface), bone under the cartilage, joint capsule, ligaments and tendons.
What are the Most Common Causes of Osteoarthritis?
Osteoarthritis in dogs usually has a specific underlying cause and is therefore often seen earlier in life. Underlying causes can include developmental conditions such as hip dysplasia or cruciate ligament rupture and injuries to the joint. Cats are very commonly affected and this may be seen at a young age.

How is Osteoarthritis Diagnosed?
The key signs or symptoms of osteoarthritis are stiffness, lameness and pain especially after rest or exercise. Joint pain associated with osteoarthritis may manifest in a number of ways, including moaning, restless sleep and altered behaviour (including aggression). Joints affected with osteoarthritis are often thickened with a restricted range of movement. Muscles on the affected leg are often reduced in size. X-rays are the most common method of diagnosing osteoarthritis and ruling out other possible causes of joint pain and lameness.
As with people, more advanced imaging (MRI, CT and ultrasound scans) is occasionally necessary. Arthroscopy (keyhole surgery) is a technique that enables inspection of the inside of joints with a camera and may be indicated in select cases, for example to detect torn ligaments. Collection and analysis of joint fluid can be important in some cases to rule out other possible causes of joint pain.
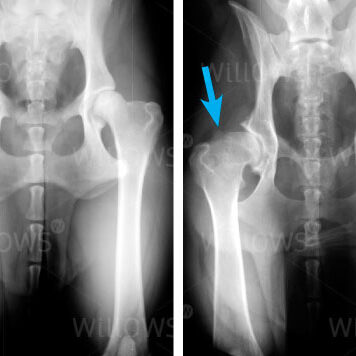
Fig 1: X-rays showing normal hip joints and hips with osteoarthritis (arrows)
What Treatments are Available for Osteoarthritis?
Unfortunately there is no cure for osteoarthritis. Treatment aims to allow pets to use the affected joint or joints without pain. There is no single approach to treatment that is successful in every case, and most dogs and cats need a multi-modal approach, including:
- Pain relief: osteoarthritis can be painful, and so in some animals long term medication is needed. Although long term medication can have a risk of side effects, this risk must be balanced against pain from the osteoarthritis if the medication is not given.
- Exercise: whilst exercise can cause discomfort in the short term, exercise is important to keep pets fit and healthy. There is no golden rule as to how much exercise an animal with osteoarthritis can have, as all patients are different; instead, exercise levels need to be tailored to the individual animal.
- Weight control: pets that are an ideal weight have fewer painful episodes and slower progression of osteoarthritis than overweight animals
- Food supplements: glucosamine, chondroitin and green lipped muscle extract have been proposed to help treat osteoarthritis. While the effect may not be dramatic small improvements may be seen
- Diet: diets containing omega-3-fatty acids may have a natural anti-inflammatory action which may help to relieve discomfort associated with osteoarthritis
- Therapy: physiotherapy and hydrotherapy are important in the treatment of osteoarthritis. They can be used to build muscle, improve joint use, and reduce muscle stiffness as well as being good exercise. These therapies need to be discussed carefully with your Vet initially, to avoid making painful joints worse.
What can I Expect if my Pet is Treated for Osteoarthritis?
Osteoarthritis is a waxing and waning disease and so animals can have good days and bad days. If symptoms of pain seem to worsen, it may be necessary change treatment and use different medications.
In some animals osteoarthritis can be so severe that medications and physiotherapy are ineffective. In these cases ‘salvage’ surgery may be considered. Arthrodesis (fusion of a joint) is often performed for the ‘wrist or ankle. Joint fusion is occasionally performed for other joints such as the shoulder, elbow or knee. In the hip, the painful ball part of the joint can be removed, an operation called an excision arthroplasty. For the hip, knee and elbow total joint replacement surgery can be considered. These are relatively big operations but animals can regain excellent, pain-free use of a limb and have a very good quality of life, especially following hip and knee replacements.
To save this page as a PDF, click the button and make sure “Save as PDF” is selected.
Orthopaedics
Find out more
To assist owners in understanding more about Orthopaedics we have put together a range of information sheets to talk you through the some of the more common orthopaedic conditions seen and treated by our Specialists.

