Why Should I Bring my Pet to Willows for Treatment of Cataracts?
Willows is one of Europe’s leading small animal referral centres. Our state-of-the-art hospital is led by internationally renowned Specialists, committed to providing the highest standards of veterinary care. Our team of Ophthalmic Specialists have a collective experience of treating hundreds of patients with cataracts.
Our Ophthalmologists are supported by our multi-disciplinary team of Specialists across a number of disciplines including; Anaesthesia, Diagnostic Imaging and Emergency and Critical Care. Willows also has a large dedicated team of Nurses and clinical support staff available 24 hours a day, every day of the year to provide the best possible care for your pet.
What is a Cataract?
The lens of the eye is located deep inside the eye just behind the coloured part (i.e. the iris). A cataract is a clouding or opacity in the lens, which makes it look white. Cataracts often form in both eyes and frequently become worse. However, one eye can be more affected than the other, in the first instance.

What are the Most Common Causes of Cataracts?
In most cases the reason a cataract develops remains unknown. Cataracts are common in older dogs and sometimes occur due to other problems such as diabetes or disease in the back of the eye (the retina). For some patients cataracts are an inherited condition.
Fig 1: A mature cataract in a dog
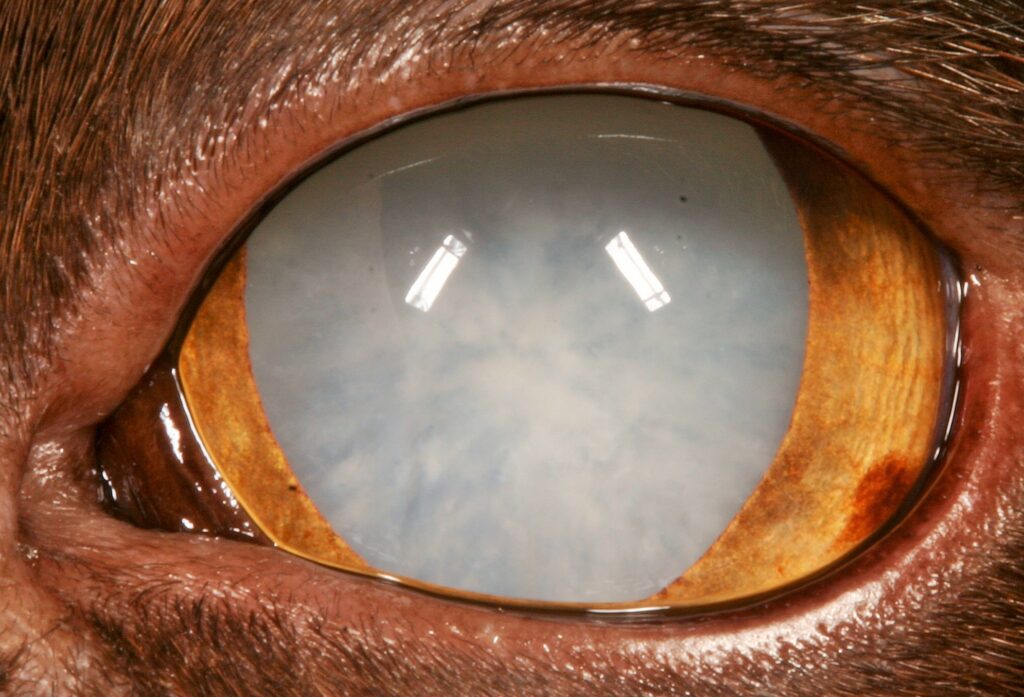

How are Cataracts Diagnosed?
In patients that have developed cataracts typical findings include the presence of opacifications on the lens associated with loss of vision. A full ophthalmic examination by an Ophthalmic Specialist will confirm the diagnosis, appropriate treatment will then be discussed with the pet owner.
Fig 2: A mature cataract in a diabetic dog – note the multiple small vacuoles
What Treatment is Available for Cataracts?
At present the only treatment for cataracts is surgery. Unfortunately, not every cataract is suitable for surgical treatment, as such it is necessary for the Ophthalmic Specialist to assess each patient and determine what therapy is possible. Some cataracts are more complicated to treat than others, a Specialist will be able to provide guidance depending upon the circumstances of each patient.
Early cataract surgery is recommended in order to avoid the detrimental effects of intraocular inflammation. Surgery is usually carried out once a cataract starts to interfere significantly with vision. This is particularly important for young and diabetic patients, where the development of cataracts can often be rapid and result in significant complications if treatment is delayed. Cataracts in older patients with very slowly progressive cataracts may be monitored, however the prophylactic use of anti-inflammatory drugs is often recommended in such cases.
Fig 3: An immature cataract in a dog which was already causing visual deficits

What can I Expect if my Pet is Treated for a Cataract?
Patients are usually admitted on the morning (or day before) of surgery. Diabetic patients require special management, and this should be discussed with the Vet involved.
Before surgery all patients have an ultrasound scan to check for problems such as retinal detachment or rupture (bursting) of the lens, and an electroretinogram (ERG) will be carried out to confirm that the retina works properly. These tests are performed under sedation. Some patients may be found to be unsuitable for surgery after the ultrasound scan and ERG are carried out.
Cataract surgery is performed under general anaesthetic, a muscle relaxant is also given so that the eye comes into the correct position for the operation. The operation is very delicate and involves the use of an operating microscope and special surgical instruments. The cataract is removed using a technique called phacoemulsification, also used in the removal of cataracts in humans. For most patients it is possible to put in an artificial lens where the old lens was. The lenses used are made specifically for each species i.e. dogs or cats. Sometimes, for technical reasons it is not possible to implant an artificial lens and the result of this is similar to someone who wears glasses not putting them on.
Most patients will stay in hospital overnight and then discharged the following day, provided progress is satisfactory. Most animals will be able to see something on the day after surgery it then often takes a few weeks for vision to settle as the eye adjusts to the effect of surgery and the presence of the lens implant.
Intensive aftercare is required following cataract surgery, often with the use several types of eye drops. The most frequently applied drops are initially used six times a day, the number of applications gradually decreases over the next two months.
Pets need to be kept as calm as possible for a few weeks after the surgery, although naturally this can be difficult. Pulling on a lead should be avoided for several weeks, to avoid increasing the pressure inside the eye and can encouraging bleeding. To avoid pulling on the lead a harness can be used. Patients will need to wear a plastic collar for approximately three weeks after the operation. Some patients, especially those with complicated cataracts, may need longer term treatment and additional check-ups. These checks take place at Willows, as the close monitoring of patients is very important in obtaining the best possible long-term result.
The success rate of cataract surgery in dogs is approximately 90%. A small percentage (10%) of patients cannot see in the operated eye after surgery, there are a number of reasons for this including: inflammation, infection, wound breakdown, bleeding, increased intraocular pressure, corneal ulcers, retinal detachment, poor vision and “after-cataract” (i.e. a white membrane that can grow across the pupil inside the eye).
The success rate of cataract surgery in dogs is high, and the great majority of patients do very well after their operation. Whilst this is a major surgery, it is one of the most commonly performed procedures at Willows and our Specialist team will be on hand to provide as much help and support as possible.
To save this page as a PDF, click the button and make sure “Save as PDF” is selected.
Ophthalmology
Find out more
To assist owners in understanding more about Ophthalmology we have put together a range of information sheets to talk you through the some of the more common conditions seen and treated by our Specialists.

